If you’re using birth control or considering it, make sure you know the dangers behind these little pills. Often, birth control pumps your body with synthetic chemicals that can cause long-term damage and even mask symptoms that are telling a bigger story.
Birth control contraceptives have become so common that their uses run well beyond that of just preventing pregnancy. Acne control, prep for fertility treatment, and managing long or irregular periods are just some of the other prescribed uses of various birth control methods.
However, birth control isn’t as safe as was once thought, and it can lead to serious and significant problems down the road. Here we will go over the health risks of taking birth control and alternative options for managing your needs.
Struggling to lose weight? Unable to focus? Chances are, your hormones are out of whack.
Grab Our FREE Guide To Fixing Your Hormones By Clicking Here!
6 Forms of Hormonal Birth Control

There are more than 60 million women of childbearing age in the U.S. 62 percent use contraceptives regularly, while 67 percent of these women using regular contraception rely on non-permanent, hormonal methods, like birth control pills, patches, implants, injectables, and vaginal rings. (1)
Different forms of hormonal birth control all have the same objective, while differing slightly in side effects and benefits.
Pills
The most common form, birth control pills, come in two primary forms: combination packs, which utilize synthetic estrogen and progestins, and minipills, which are progestin only. (2)
With combination pills, you can essentially choose how many periods you want to have per year, with common packs allowing for monthly cycles or extended cycles (periods four times a year). Formulations that completely eliminate periods altogether are also available. Combination pills come with higher risks, but these progestin-only pills do not fully prevent ovulation.
Combination pills come with higher risks, so minipills are sometimes recommended, but these progestin-only pills do not fully prevent ovulation. Instead, they thin the uterine lining and thicken cervical mucus to prevent the released egg from fertilizing.
Patches
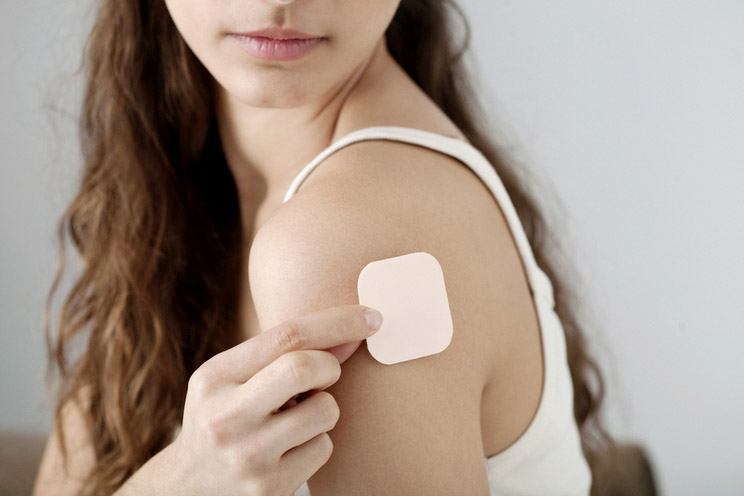
Delivering the same hormones as the combination pill, patches are worn on the abdomen and deliver hormones via skin absorption. It is replaced once a week at the same time for three weeks, and then discontinued the fourth week to allow a period to come. (3)
Implants
Progestin-only implants are placed in the upper inside of the arm and work like minipills. While they don’t prevent ovulation, they have a failure rate of 0.05 percent. (4) They do, however, come with some side effects and some strong contraindications, such as not being recommended for women with current or past breast cancer, a history of heart disease or stroke, antibodies for lupus, history of migraine with aura, or liver problems due to the high potential for severe consequences.
Injectables
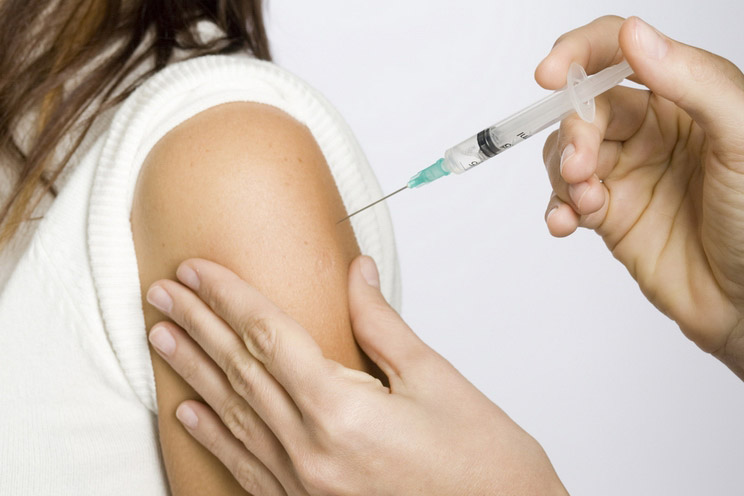
Injectable birth control is another progestin-only option that is injected either subcutaneously or intramuscularly every three months by a provider. (5) While it is considered safer for women who cannot take estrogen birth control options, injection birth control comes with some hefty risks, including delayed return of fertility (10+ months before normal ovulation returns) and bone density loss. (6)
Vaginal Rings
Vaginal rings are combination methods of birth control that are placed inside of the vagina and deliver hormones for three weeks. Each ring is discarded after three weeks to allow a period to come, and then a new ring is inserted. This can be done by the patient at home, no provider visit necessary. (7)
IUD
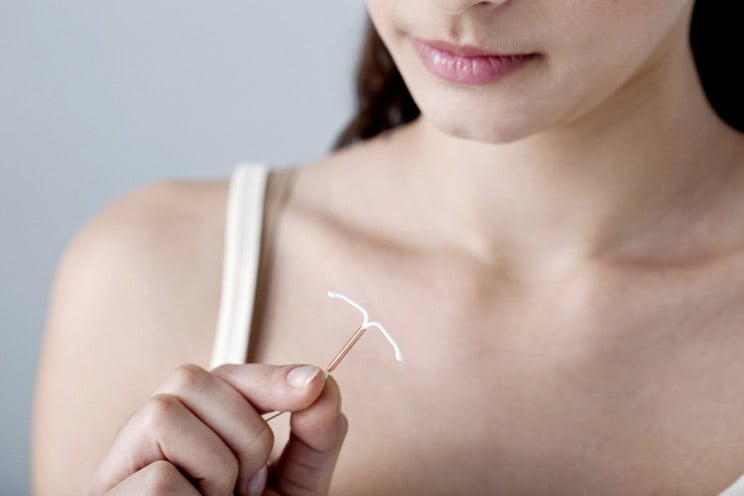
IUD, short for intrauterine device, is a small, T-shaped plastic device that is inserted vaginally by a provider. It delivers progestin-only hormones. (8) Hormonal IUDs work longer than other forms of hormonal birth control, and are the only long-lasting, non-permanent form of contraception. Most last between three to five years.
Bottom line: While there is no shortage of hormonal birth control options, all of them carry weighty risks. Even minor side effects, like mood disorders or weight gain, can be enough to significantly disrupt one’s quality of life.
6 Dangers of Hormonal Birth Control
We’ve been inundated with views that it’s normal to take birth control, but when we, the women whose bodies are being pumped full of synthetic hormones, take a step back and consider the big picture, do we really want to sign on this dotted line?
1. Infertility
Many women are finding that years of birth control use significantly delay or damage their fertility, often resulting in longer times to conception, increased risks of miscarriage or ectopic pregnancy, or the need for assisted reproductive technology, like IVF. (9, 10, 11, 12)
Nearly all forms of hormonal birth control carry side effects of weight gain, which can be significant, and weight or obesity factors can also independently lead to fertility problems or the inability to conceive. (13)
2. Blood Clots, Blood Pressure, Stroke, and Heart Attack

While numerous factors (such as smoking) can affect a woman’s risk of blood clots, combination pills at least double the risk of having a blood clot in a vein. (14)
Many forms of birth control carry a potential side effect of raising blood pressure. When you factor in other causes of increased blood pressure, like genetics, age, smoking, or obesity, some women will face substantially higher chances of encountering a blood pressure related issue, like stroke or heart attack, or even preeclampsia later if a pregnancy is achieved.
The risk for heart attack using certain forms of birth control increases for all women, even those who don’t have genetic clotting disorders, which can also independently increase risk. (15)
3. Yeast Overgrowth
Birth control, especially long-term use, disrupts the normal flora of the vagina, and can lead to increased occurrences of yeast infections. (16) When candida, the bacteria that is commonly referred to as yeast, becomes a regular problem, it can overgrow into other areas of the body, particularly the intestines, leading to chronic candidiasis and other health problems, like chronic fatigue. (17)
4. Cancer

Hormonal birth control can lead to an increased risk for two forms of cancer: ovarian and breast. (18, 19, 20) Beyond that, IUDs specifically carry an increased risk of developing ovarian cancer. (21)
Note: Women are exposed to many daily factors that can increase a risk of female reproductive disorders and cancers that go well beyond a daily dose of birth control, including xenoestrogens in plastic products, cosmetics, and skincare products.
5. Mood Disorders, Including Depression and Anxiety
Birth control increases the elimination of water-soluble B vitamins, which have a strong neurological and mood impact. (22) Combination birth control methods that use estrogen can increase a chance for mood disorders, including depression. (23, 24)
6. Sex Drive

A common side effect of many forms of hormonal birth control includes a decreased sex drive. (25) Reduced sex drive while on birth control can also be tied to the other common birth control side effects like weight gain, breakthrough bleeding, acne, fatigue, and breast tenderness, all of which can quickly kill the mood for sex.
Additional Risks of Hormonal Birth Control Include: (26, 27, 28, 29, 30)
- Abdominal pain
- Absence of periods
- Acne
- Bone density loss
- Breakthrough bleeding
- Breast tenderness or pain
- Cramping or pelvic pain
- Cysts on the ovaries
- Decreased libido
- Delayed return of fertility
- Diarrhea
- Dizziness
- Endometrial or cervical cancer
- Endometritis (endometrial inflammation)
- Fatigue
- Fluid retention
- Gallbladder problems or disease
- Headaches
- Increased blood pressure
- Increased risk of ectopic pregnancy
- Increased vaginal fluids
- Irregular, prolonged, or frequent menstrual bleeding
- Liver cancer or tumors
- Nausea
- Nervousness
- Ovarian cysts
- Pelvic infections
- Skin irritation
- Toxic shock syndrome
- Vaginal infection or irritation
- Weight gain
6 Healthier Alternatives
1. Male Condoms

Perhaps the most common non-hormonal method of birth control, condoms are cheap, convenient, and simple to use. Hormonal birth control options don’t protect against STDs, and condoms do, so these have an added level of protection.
Success rates of condoms are 98 percent when used correctly. (31) One thing some fail to consider: condoms have expiration dates, and should be replaced regularly to ensure that they function as they should. Hormonal birth control options don’t protect against STDs, and condoms do, so these have an added level of protection.
Another factor to consider with condoms is the materials they’re made from. Most condoms on the market are made from latex, but other latex-free alternatives exist that are made from polyurethane or polyisoprene. Still, if you’re looking to find a more naturally-made substance, some companies produce lamb skin condoms. Note: While lamb skin condoms can have less irritating reactions, they do not protect against STDs.
2. Female Condoms
Less common than male condoms, female condoms don’t have quite as high of a success rate (79 percent). They are also a little less easy to use, and can cause vaginal irritation. But they do protect against sexually transmitted infections, and they are an option if male condoms don’t work.
3. Spermicide and Diaphragm or Cervical Cap

Similar to a female condom, the diaphragm or cervical cap must be inserted to fully cover the cervix. On their own, they’re about 80 percent effective, but this can increase with the use of a spermicide to ensure that sperm that do make it past the barrier don’t go on the fertilize an egg. (32)
These options are less convenient since it can require some effort to get into place, and occasionally, can get stuck inside of the vagina. It also requires a prescription and a fitting. They can’t be used during a period, either.
4. Nonhormonal IUD
While hormonal IUDs carry a load of side effects, copper IUDs contain no hormones and carry less risk. They are longer lasting and can remain implanted for up to 10 years. They do have the potential to increase heavy bleeding during periods, since they don’t interfere with ovulation or normal menstrual cycles. They also have a slight chance of coming out, or slipping out of place and not preventing pregnancy, but they have a 99 percent success rate. (33)
5. Natural Family Planning
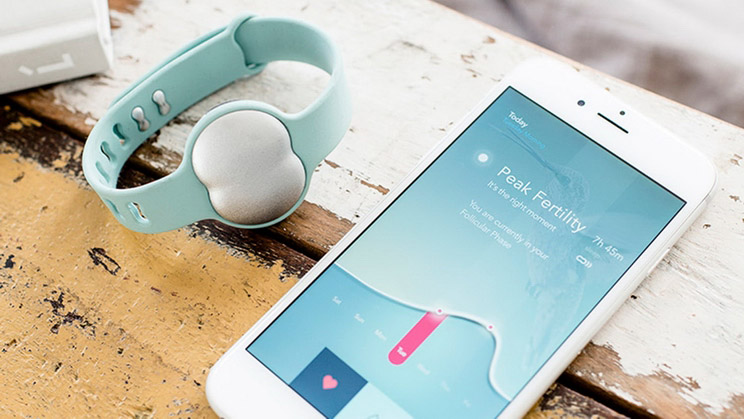
This form of birth control is the one that most truly preserves natural fertility and reduces exposure to synthetic hormones, barrier methods, and implants. While it’s really only ideal for partners in committed partnerships (since it doesn’t protect against STDs), it can present the most freedom.
With the advance of the smartphone, most women can track their fertility in an app using simple measurements like taking a daily morning temperature or monitoring cervical fluid around ovulation. Generally, women will need to avoid intercourse for 7-10 days each cycle. If you properly track your fertility signs, this method can be very effective. The true bonus is that it can be turned around and used to achieve pregnancy quickly if you do decide that you want to conceive. Hormonal methods of birth control disrupt ovulation and once stopped, can still lead to long wait times before conception. Other devices, like the Ava bracelet, are worn around the wrist while you sleep, and can pinpoint fertile days with 89 percent accuracy.
If you really want to get high-tech with your natural pregnancy avoidance, there are devices designed for tracking natural fertility. While they’re aimed at improving a woman’s odds of conception, they come with high success rates of identifying fertile windows. If you identify when you’re capable of getting pregnant, you can easily avoid pregnancy as well.
Some of these devices, such as the Ovusense and Ovacue, are inserted in the vagina while you sleep, and provide real-time updates on fertility. Other devices, like the Ava bracelet, are worn around the wrist while you sleep, and can pinpoint fertile days with 89 percent accuracy.
6. Sponge
Similar to a cervical cap, a sponge filled with spermicide is inserted into the vagina. It is more effective for women who haven’t already had children, since a widened vaginal canal from giving birth can lead to a nearly 25 percent failure rate for this method. Women who have never had a child will still have around a 10 to 12 percent of pregnancy while using the sponge, making it less successful than other methods. In rare cases, it can be difficult to remove.
Bottom line: Numerous alternatives to hormonal birth control exist, varying in degrees of effectiveness. The form of birth control you choose should best meet the needs of your health goals. When weighing the risks of hormones, non-hormonal options can be as effective and even empowering, since they don’t suppress a woman’s natural fertility, mood, or vibrant health.

(Read This Next: Paleo and Hormone Balancing)



 Whatever-You-Have Crockpot Soup Recipe
Whatever-You-Have Crockpot Soup Recipe









Show Comments